How Is Healthcare Quality Ensured in Nepal Peer Review
- Research article
- Open Access
- Published:
Factors affecting institutional delivery in rural Chitwan district of Nepal: a customs-based cross-sectional study
BMC Pregnancy and Childbirth book 15, Article number:27 (2015) Cite this article
Abstract
Background
Health facility delivery is considered a critical strategy to improve maternal health. The Government of Nepal is promoting institutional delivery through dissimilar incentive programmes and the establishment of birthing centres. This study aimed to identify the socio-demographic, socio-cultural, and health service-related factors influencing institutional delivery uptake in rural areas of Chitwan district, where high rates of institutional deliveries co-exist with a significant proportion of home deliveries.
Methods
This community-based cross-sectional study was conducted in six rural Village Development Committees of Chitwan commune, which are characterised by relatively depression institutional commitment rates and the availability of birthing centres. The study area represents both hilly and plain areas of Chitwan. A full of 673 mothers who had given birth during a 1-yr-period were interviewed using a structured questionnaire. Univariate and multivariable logistic regression analysis using stepwise astern emptying was performed to identify central factors affecting institutional delivery.
Results
Adjusting for all other factors in the final model, advantaged degree/ethnicity [aOR: i.98; 95% CI: 1.fifteen-3.42], support for institutional delivery by the husband [aOR: 19.85; 95% CI: 8.53-46.21], the conclusion on place of delivery taken jointly past women and family members [aOR: 5.43; 95% CI: ii.91-10.16] or by family members alone [aOR: 4.61; 95% CI: two.56-8.28], nativity preparations [aOR: 1.75; 95% CI: i.04-2.92], complications during the well-nigh recent pregnancy/delivery [aOR: 2.88; 95% CI: ane.67-4.98], a perception that skilled health workers are e'er available [aOR: 2.lxx; 95% CI: 1.20-6.07] and a birthing facility located within one hour's travelling distance [aOR: 2.15; 95% CI: 1.26-three.69] significantly increased the likelihood of institutional delivery. On the other mitt, not knowing most the adequacy of concrete facilities significantly decreased the likelihood of institutional delivery [aOR: 0.14; 95% CI: 0.05-0.41].
Conclusion
With multiple incentives present, the conclusion to deliver in a health facility is affected by a complex coaction of socio-demographic, socio-cultural, and wellness service-related factors. Family unit decision-making roles and a husband'southward back up for institutional commitment exert a particularly strong influence on the identify of delivery, and this should exist emphasized in the health policy as well every bit development and implementation of maternal health programmes in Nepal.
Background
Improving maternal health is one of the United Nation's Millennium Evolution Goals (MDG 5) with a target of reducing the maternal mortality ratio (MMR) past iii quarters by 2015 from its 1990 level [1]. Globally, 289,000 maternal deaths occurred in 2013. Near all the maternal deaths (99 percent) occurred in developing countries [two]. Continuous care during pregnancy, delivery and the postpartum period is essential for maternal and newborn wellness. The virtually risky catamenia for mother and child is during child nascence and the offset few days postpartum [3]. Between 1996 and 2006, the MMR in Nepal dropped from 539 to 281 per 100,000 live births [4] and to 190 per 100,000 live births in 2013 [2]. However, the MMR of Nepal is still highest in the S Asian countries except Transitional islamic state of afghanistan [2].
In a land similar Nepal, the chances of a safety delivery are greater when the birth takes place in a wellness facility than at domicile, and increasing institutional delivery is important to reduce deaths due to pregnancy complications [five,6]. Although there has been a meaning rising in institutional commitment in the past 10 years, with an increase from nine percent in 2001 to 35 per centum in 2011, about ii thirds of births in Nepal (65 per centum) keep to take place at home [7]. Thus, encouraging institutional delivery and 24-hr emergency obstetric care services at selected public health facilities in every district is i of the major strategies Nepal has adopted to reduce the adventure of dying during childbirth [8]. A safe birth includes providing supportive company, ensuring make clean commitment practices, every bit well equally early detection and management of maternal and neonatal complications. Life-saving packages consisting of medications and surgical material should be available at every birth and admission to operative vaginal delivery, to caesarean section, and to claret transfusion should be within a reachable distance [5,6]. Thus, the Nepali government has added new birthing centres within health posts/sub-health posts to increase the number of institutional deliveries [8]. These centers provide a 24-hour service to manage uncomplicated deliveries and to refer complicated cases to hospitals [8]. In addition, nether the Safer Mother Programme, which came into effect in 2009, handling of all deliveries with or without complications is provided free of accuse at all those governmental, individual as well as NGO-run health facilities and teaching hospitals that have received permission from the Government of Nepal [9]. Moreover, a greenbacks incentive provided to mothers after having given birth at a health facility forms part of a safe delivery incentive program since 2005 [8]. Additionally, in programmes such as the Customs Based Newborn Care Program (CB-NCP), female person community health volunteers (FCHVs) identify and counsel pregnant women and encourage them to deliver in a health establishment [10].
Chitwan district, the study setting, is located in the southern evidently (terai) of Nepal (with some hilly areas) and is characterized by a relatively improve health and route infrastructure than other districts. As a upshot, the percentage of institutional deliveries is much higher (83 percent) [11] compared to the nation every bit a whole (35 percent) [7]. Nonetheless a pregnant proportion of deliveries take place at dwelling, specially in rural areas. Thus, this setting is peculiarly suitable for examining the factors that favour or limit institutional delivery, and to derive lessons learnt that may exist applicable to other districts beyond the land. This written report aims to identify socio-demographic, socio-cultural, and wellness service-related factors influencing institutional delivery in rural areas of Chitwan district.
Methods
Written report setting
Geographically, Nepal is characterized by three ecological regions - mountain, hill and plainly. The country is divided into 75 districts, and each district is structured in Hamlet Development Committees (VDCs) and municipalities that are classified as rural and urban respectively [12]. Each VDC and municipality is farther divided into smaller authoritative units called wards. There are nine wards in each VDC, while the number varies for municipalities.
Chitwan commune is located 148 kilometers far from the capital Kathmandu. The district comprises a full of 36 VDCs, ix located in the hills and 27 located in the plain [eleven], and two municipalities with a total population of 579,984 [thirteen]. Co-ordinate to the National Population and Housing Census 2011, the distribution of unlike caste/ethnicities in the district is as follows: upper caste (Brahman and Chhetri) 41 percent; advantaged Janajati 12 percent; Dalit eight per centum; and disadvantaged Janajati 39 pct [14]. About two thirds of the population aged five years and above are literate, with three quarters of males compared to 57 percent of females [15]. One third of males do not live at home, with most of these working away [15]. A composite alphabetize based on poverty and deprivation, socio-economic and infrastructural development, and women's empowerment shows Chitwan to exist the 2d well-nigh developed commune in Nepal [16].
At that place are several hospitals in Chitwan: one government sub-regional hospital, two teaching hospitals and 36 private hospitals. Nigh of them are located in the district headquarter Bharatpur and with birthing facilities. In rural areas, wellness services are provided through four primary health care centers (PHCCs), 24 health posts (HPs) and 12 sub-health posts (SHPs) [eleven].
Study blueprint, study participants and sample size
This customs-based cross-sectional study included all women who had given nativity during the one-year menstruum between Apr 21, 2012 and April 20, 2013 (i.e. one week prior to the start of data collection, which allowed FCHVs i week to tape the nascence).
First, six rural VDCs - 3 hilly (Kaule and Chandivanjyang with birthing centres and Kabilas without a birthing center) and 3 plain (Piple and Ayodhyapuri with birthing centres and Padampur without a birthing centre) VDCs - were selected on the footing of a lower-than-district average pct of institutional commitment and the availability of birthing facilities. In the six selected VDCs, the full female population of reproductive age (fifteen–49 years) was 17,690 and the expected pregnancies were 1891 [11]. Secondly, in each VDC, six out of ix wards were selected randomly, with two thirds of wards assumed to exist representative of the VDC as a whole and generating a sufficiently large number of deliveries. Finally, at ward level, all mothers having given nascence during the specified one-year-period and residing in the ward were interviewed. The sampling process is shown in Effigy 1.
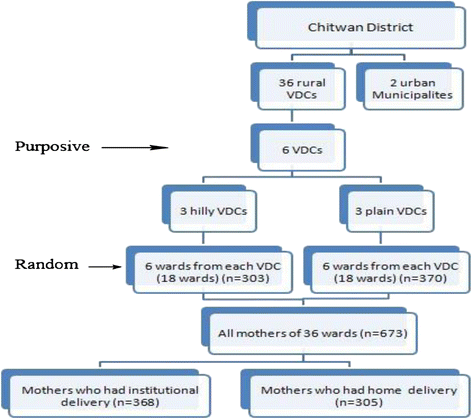
Sampling procedure and sample size.
The sample size for the study was calculated with the average 46 percent prevalence of institutional delivery of the vi selected VDCs as reported past the CB-NCP [unpublished observation], four pct margin of error, and assuming a non-response rate of 10 percent. This resulted in a final sample size of 663, allowing for sufficient ability even in view of the many questions asked through the survey [17]. Altogether 673 mothers were included, amidst whom 368 had delivered at a health facility and 305 had delivered at home (Effigy 1).
Data collection
Data collection took place between Apr 26, 2013 and June 30, 2013. Chitwan is one of the districts where the CB-NCP is implemented. FCHVs keep a tape of all meaning women and mothers who have given birth. The FCHVs of the selected wards were visited at their homes and a list of mothers who had given nascence between Apr 21, 2012 and April twenty, 2013 was developed from their records. In addition, other eligible mothers of the written report area not reached by the FCHVs, primarily due to geographical or distance reasons, were also included in our written report. These were identified by asking the FCHVs themselves, as well as other local residents.
A structured questionnaire was prepared in the local Nepali language on the basis of a review of the relevant literatures and the preliminary analyses of separately conducted focus group discussions and in depth interviews (manuscript in preparation). The questionnaire included socio-economic, demographic and cultural variables related to the role of family and neighbours, variables related to perceived demand for health care, and wellness service-related variables. It was pre-tested among 35 women residing in 3 other rural VDCs of Chitwan commune that are similar to those of the written report area. The feedbacks from the pre-examination were incorporated and questionnaire was then finalized. Modifications included a re-ordering of questions as well every bit changes in words and additions/deletions of some reply categories.
Data drove took place through face up-to-face interviews with the participating mothers by visiting them at their homes. Eight experienced enumerators, Bachelor students of public wellness and Master students of sociology, were selected to collect the data. For two VDCs, the enumerators were recruited locally, while for the other VDCs most of the enumerators were not local residents merely familiar with the area. The first writer provided them with two days' training, and they were also involved in the pretesting of the questionnaire.
Variables
Table 1 shows the structure of dependent and contained variables in major groups (i.e. socio-economic and socio-demographic variables, socio-cultural factors including the role of family and neighbours and perceived need-related variables, perceived health service-related variables and distance to birthing facility); where needed, additional description of variables is provided. The dependent/outcome variable, i.e. place of delivery, assesses whether the most recent child birth occurred at a health institution (coded 1) or at abode (coded 0).
Caste/Ethnicity
The caste-ethnicity variable reflects the important socio-cultural structure of Nepali gild [18-xx]. The hierarchical degree system is cardinal to the Hindu faith. Upper caste Hindus (e.g., Brahman and Chhetri) are at the pinnacle of the social hierarchy and are presumed to be socio-culturally, economically and politically advantaged compared to other caste/ethnic groups [20,21]. Historically, Dalits (e.g., Kami, Sunar, Damai, Sarki) are untouchables and positioned at the bottom of the social hierarchy. Janajatis (e.g. Gurung, Tamang, Magar, Newar) may also have hierarchy inside their organisation, but the social bureaucracy is not as distinct as in other degree groups. The upper degree Hindu and Newar people are among the historically privileged groups and are considered the elites [20,22]. It is believed that these groups, particularly the upper caste Hindu, have the best admission to various economical and not-economic opportunities [23].
The Ministry building of Health and Population of Nepal has classified the different degree/ethnicities into 6 categories: upper degree group (Brahman/Chhetri), relatively advantaged Janjatis, disadvantaged Janjatis, disadvantaged non-Dalit terai caste group, Dalits, and religious minorities [24]. In the present study, the caste/ethnicity variable was dichotomized into an advantaged group (i.e. upper castes (Brahman/Chhetri) and advantaged Janajatis) and a disadvantaged group (i.e. disadvantaged Janajatis, Dalits, and religious minorities) [25].
Wealth index
A wealth alphabetize was created using a principal component analysis of a number of household assets [26], i.e. possession of a radio, television, mobile, other kind of phone, and lookout man; dwelling characteristics - material of roof and wall of firm, availability of a toilet, type of toilet and access to drinking water and electricity. The gene score from the showtime component of the chief component analysis was used to classify respondents with poorer and ameliorate wealth index.
Education
Education is measured in 3 categories - no education, primary and secondary. Women who had completed whatsoever of the grades from 1 to 5 were classified every bit having primary instruction. Women who had completed six grades or more were classified equally having secondary or higher education.
Nativity order
The club of the contempo birth was categorized as 'first' , 'second or third' , 'quaternary or more'.
Terminal decision-maker
The final decision regarding place of delivery was categorized as adult female alone, adult female and family unit members jointly and family unit members and FCHVs. The FCHV category was merged with other family members as its frequency was very low, i.e., four out of 673.
Back up of hubby
This variable assessed verbal or physical support by the husband towards institutional delivery, such as carrying the woman to the wellness facility, arranging for transportation, or saving money.
Support of neighbours
This variable assessed verbal or physical support by neighbours towards institutional delivery, such as help in carrying the woman to the health facility.
Birth preparation
Women were considered prepared for birth when at least one of 5 components of birth preparation, i.e. saving money, arranging transportation, identifying health institution and contacting a health worker, identifying a person who can donate blood in instance of demand, and owning a clean delivery kit [7], had been accomplished.
Number of antenatal care (ANC) check-ups
The number of antenatal care check-ups a woman had during her contempo pregnancy was counted. The response is grouped as – no visits, less than 4 visits, and 4 or more visits.
Experience of complications
Perceived experience of complications during the recent pregnancy or childbirth measured every bit a dichotomy (yes = 1; no = 0).
Availability of skilled health worker
This variable measures how women perceived the availability of skilled health workers at the nearest birthing facility (a birthing center or hospital).
Care and respect from health workers
This variable measures how women perceived the care and respect of the health workers at the nearest birthing facility.
Availability of drugs and equipment
This variable measures the perceived availability of the necessary drugs and equipment at the nearest birthing facility.
Adequacy of physical facilities
This variable measures the perceived adequacy of the physical facilities/infrastructure at the nearest birthing facility including a waiting room, a bed room, a room for delivery, calorie-free and water.
Distance to birthing facility
The distance to the birthing facility is measured as the time required to reach the nearest birthing facility with the available means of transportation, whether by vehicle, bamboo basket, and hammock or past walking.
Data processing and assay
Information entry was undertaken in Epi data version 3.i [27]. Analyses were conducted in SPSS version sixteen [28]. The event of involvement was place of delivery, coded every bit a binary variable. We initially conducted univariate logistic regression analyses to obtain unadjusted odds ratios for the event of a broad range of variables on institutional delivery. We then used multivariable logistic regression assay and stepwise astern elimination, where all contained variables are entered in the initial model and at each step the variable with the to the lowest degree significance (the highest p-value greater than 0.05) is eliminated. The final model, which is the reduced model, included all the variables showing significant associations with place of delivery [29].
To diagnose potential multi-collinearity bug among the independent variables, a collinearity diagnostic exam available in SPSS was used. A tolerance statistic above 0.2 and a variance aggrandizement factor (VIF) value above 5.0 were considered to indicate multi-collinearity [30]. All the same, all the VIF values were well below 3.0.
Upstanding considerations
The Nepal Health Inquiry Council granted upstanding clearance to carry out this written report. Nosotros obtained a written permission from the District Public Health Role in Chitwan to implement this study in Chitwan. An informed consent form was prepared on the basis of templates fabricated available by the World Health Organization (http://www.who.int/rpc/research_ethics/informed_consent/en/). Prior to the kickoff of the interviews, nosotros obtained exact consent from the respondents as virtually of them were illiterate. Exact informed consent was obtained from the women or from their guardian/parent/next of kin if the women'southward age was below the legal historic period, for the publication of this report and whatever accompanying images.
Results
Description of written report participants
Amidst the 673 women participating in the study, 55% (n = 368) had delivered at a health facility and the remaining 45% (n = 305) had delivered at dwelling (Table 2). This institutional delivery rate is significantly beneath the boilerplate for Chitwan district (83%), which is a direct consequence of the confinement of the study area to rural areas.
Table ii as well shows the distribution of independent variables. Among the socio-economic and socio-demographic factors, a college proportion of younger women living in VDCs in plainly areas, of advantaged caste/ethnicities, with better wealth alphabetize and having secondary or higher education gave nascency at a health facility. Similarly, as expected, the percentage of institutional commitment decreased with increasing birth lodge. With respect to the role of family and neighbours, women who were encouraged to deliver at a health institution past their husbands were more likely to do then than women who were not encouraged by their husbands. However, unexpectedly, those women who decided on place of commitment by themselves were more likely to deliver at home. With respect to perceived need, a college proportion of women who had prepared for birth, had had antenatal check-ups or experienced complications during the electric current pregnancy/delivery gave birth at a health facility. Similarly, a higher proportion of those women who reported that wellness workers were always available, always care and respect patients, and that drugs and equipment were ever available, and physical facilities were acceptable gave nascence at a health facility. More than women living within ane hour's distance gave birth at a wellness facility.
Multivariable analysis
Table 3 shows the results of univariate and multivariable logistic regression. In univariate models, all variables were statistically significantly associated with the outcome. Still, adapted odds ratios from the multivariable assay are reported only for those variables that are statistically significantly associated with the place of delivery and are included in the final model.
Of the various socio-economic and socio-demographic variables in the analysis, only the result of caste/ethnicity remained statistically significant in the multivariable analysis. Adjusting for the consequence of all other variables in the final model, mothers of advantaged caste/ethnicity were almost two times (adjusted OR i.98; 95% CI one.15-3.42) more probable than mothers of disadvantaged caste/ethnicity to deliver at a health facility.
Interestingly, mothers were more likely to deliver at a health facility if the decision was taken jointly by the mother and family members [aOR: v.43; 95% CI: 2.91-10.16], or by other family unit members and/or FCHVs [aOR: 4.61; 95% CI: ii.56-8.28] compared to the determination taken by the women alone. Encouragement from the husband was very important for the conclusion. Mothers who were supported by their husbands to evangelize at a health facility beingness about 20 times [aOR: 19.89; 95% CI: 8.53-46.27] more probable to deliver at the health facility compared to those whose husbands did not encourage them to do and then.
Of all the perceived need-related variables only birth preparation [aOR: 1.75; 95% CI: ane.04-ii.92] and the experience of complications during pregnancy or childbirth [aOR: 2.88; 95% CI: one.67-4.98] had increased the odds of institutional delivery in the last model.
Among the perceived wellness service-related variables, but the availability of skilled wellness worker and the adequacy of physical facilities retained in the final model. Women believing that skilled health workers were always bachelor were about 3 times [aOR: 2.70; 95% CI: one.20-6.07] more likely to deliver at a wellness facility compared to those who perceived the health worker to be sometimes available, net of all other factors. Those who had no thought about the adequacy of the physical facilities of the wellness facility were far less likely to evangelize there than those who perceived the health facility infrastructure to be inadequate [aOR: 0.fourteen; 95% CI: 0.05-0.41].
Plainly, those who reported that it takes less than an hour to reach the nearest birthing facility past the available means of transportation were more than than two times [aOR: 2.15; 95% CI: 1.26-three.69] as likely to deliver there compared to those reporting longer travel times.
Discussion
Significance of socio-economic and socio-demographic factors
Findings revealed that degree/ethnicity was the just socio-economic/demographic variable that statistically significantly influenced institutional delivery and retained in the terminal model. This is in contradiction to the findings of previous studies conducted in Nepal [31,32], where age, parity and education showed clear associations with institutional delivery. The reason may be that due to the mode we categorized the castes/ethnicity variable and the distribution of castes/ethnicity in the study expanse, the differences between advantaged (i.e. Brahman/Chhetri, very few Gurung and Newar) and disadvantaged (i.e. disadvantaged Janjati- Chepangs/Tamang/Rai/Tharu, and Dalits) castes/ethnicity were much more pronounced compared to other studies. Some other important reason may be that we included a specific decision-making variable (see next section), which is absent-minded from most studies [31-34]. A study conducted in India concluded that economical status was more of import for the decision on the place of delivery than fifty-fifty distance to a health facility, applicable peculiarly in private-for-turn a profit health facilities [35]. At least in the setting of our report, this observation was non supported, which is likely to be a result of the introduction of complimentary delivery services and motherhood incentives in Nepal, as well as the expansion of birthing facilities to rural areas.
Significance of the role of family in conclusion-making
Surprisingly, this study suggests that the likelihood of institutional delivery was greater when the decision on the place of delivery was taken jointly by the mother and other family members and even when other family members decided without the mother but together with the FCHV than when the mother decided by herself. Information technology suggests that a woman's autonomy alone is non a critical cistron but interacts with others, such as the fact that many husbands in the report area are absent-minded for work. Reaching a health facility can be hard and, consequently, shy and immature women may not wish to go to a health institution for delivery imposing this burden on their husbands' family. Similar findings were observed in a study in Republic of uganda [36], where the likelihood of institutional delivery was nigh half-dozen times greater when the conclusion was taken past both spouses together and near 5 times greater when it was taken together with other relatives than when the conclusion was taken past the women alone [37]. Similarly, evidence from Tanzania showed that the likelihood of institutional delivery was higher when both husband and married woman valued the importance of institutional commitment and the significance of doctors compared to traditional birth attendants [38]. Our finding also echoes that of an overview article on maternal survival, which suggests that women are reluctant to apply available services due to the difficulties in accessing transportation, people needed for company and finding it shameful to requite birth in front of others [6].
Our finding that a hubby's explicit support for institutional delivery influences the chances of a child being born at a health facility adds further weight to the significant office of the family unit in decision-making. Similar findings regarding the importance of a husband's support were obtained in studies from Tanzania [38], Bangladesh [39], and Uganda [forty]. Overall, these results suggest that the husband and other family members exercise play a significant role in the decision on place of delivery and that campaigns to encourage institutional delivery should not merely target women themselves merely as well their families.
Significance of perceived need-related factors
Our study shows that being prepared for birth (with saving coin beingness the near common exercise and other recommended preparations beingness poorly applied) and the feel of complications during the current pregnancy or childbirth significantly increased the chances of institutional delivery. The importance of birth preparedness was previously reported for Nepal [41] and Bangladesh [42], and was well emphasized in low- and middle-income countries [43]. The issue of complications during pregnancy and childbirth merits item attention, equally according to the Nepal Maternal Mortality and Morbidity Study, 41% of maternal deaths in 2008/09 occurred in a health facility (an increase from 21% in 1998) compared to 40% taking identify at home (a decrease from 67% in 1998) [44]. These numbers suggest that it is however primarily women with complications that are brought to a health facility and that many women seek care also tardily [45]. Indeed, amongst the maternal deaths that occurred in hospital in 2008/09, 83 percent were admitted every bit an emergency instance in a critical condition [44].
Unlike studies in Nepal [31,32], and Ethiopia [46,47] the nowadays study constitute no clan of ANC use with the place of commitment. Also, ANC utilise did not emerge as a critical factor influencing institutional delivery in a study conducted in Uganda [36]. One possible explanation may be the fact that the experience of pregnancy complications increases the likelihood of a greater number of ANC cheque-ups, making the latter variable redundant in the last model. In summary, efforts to strengthen institutional delivery in Chitwan and other districts of Nepal should stress the importance of beingness prepared for birth and the advantages of an institutional commitment and independent of the immediate need for help due to complications during pregnancy and childbirth.
Significance of perceived health service-related factors
A adult female's perception with respect to the constant availability of a skilled health worker and the adequacy of physical facilities was associated with a greater likelihood of institutional delivery. The international literature offers mixed results regarding the quality of health service and their influence on the identify of delivery [48,49]. While the quality of health services ever plays an important role, in a Nigerian study the competence of doctors/midwives and their 24-hour availability to provide maternity service was critical [48], while a Bangladeshi study indicated that more value was attached to the respectful behaviour of health workers rather than their technical skills [49].
In many rural communities in Chitwan the birthing facilities were but built during the last two years and go along to be characterised by very poor infrastructure and by few of their staff, mostly auxiliary nurse midwives, having received the training to go a skilled birth attendant. This may explain why women valued the quality of personnel and infrastructure more than the behaviour of health workers. Ultimately, all aspects of quality of healthcare including an adequate facility characterised past adequate rooms for adaptation, service delivery, water, light; the availability of drugs and other commodities and the provision of services at all hours by competent and respectful healthcare workers will exist critical in increasing institutional commitment rates.
Significance of distance to birthing facility
In the current report women living within i hour'due south altitude from a birthing facility were more probable to requite birth there than women living further away. This finding is consistent with another study conducted in Nepal [32], besides as studies undertaken in Tanzania [50] and Bangladesh [51]. Therefore, despite the authorities's efforts to establish facilities nearby and to provide incentives, accessibility continues to be a problem and requires further attention in programmes to promote institutional delivery.
Strengths and limitations
This study is not free from some methodological limitations but equally shows some important forcefulness. Like all cross-sectional studies, it identifies associations of different factors with institutional delivery but cannot establish causal relationships.
The study area was confined to six rural VDCs of Chitwan district, characterized by relatively low institutional delivery rates. While this may limit the generalizability of findings to other settings in Chitwan district and the country as a whole, most 3 quarters of the study population were of disadvantaged ethnicity, which is the priority group targeted by the authorities of Nepal in the provision of safe maternity services [52]. Importantly, we ensured that all eligible mothers that had given birth during a pre-defined menses were identified and recruited into the study by consulting FCHVs, reviewing their records and making additional enquiries with other local residents. The not-response rate of eligible mothers who could non exist recruited as they had gone to their maternal home, to work or could non exist accessed due to heavy rains did not exceed the 10 percent included in the sample size estimation. It is unlikely that any bias was introduced through non-responders, every bit they were of similar socio-economic status and from the same indigenous groups equally the included mothers.
Conclusions
This written report, conducted in rural Chitwan district, shows that socio-demographic, socio-cultural, and health service-related factors interact in determining the uptake of birthing facilities by significant women and their families. Ane finding worth highlighting is the critical role that husband's support plays in the determination for institutional delivery. Gender roles limiting women'due south involvement in decision-making, young women having no admission to fabric resource and higher illiteracy rates make women dependent on their husbands and other family members in having access to maternal wellness services, including delivery at a health facility. In addition, in some rural areas without an established transportation infrastructure, women accept to be carried by their husbands to achieve health facilities.
Therefore, in the geographical and socio-cultural context of Nepal, programmes to promote institutional delivery must, on the ane hand, piece of work through the empowerment of women and, on the other mitt, specifically target husbands (and, to a lesser extent, other family members) and strengthen their involvement. Other important implications for policy and practise emerging from this study are a demand to focus on families from disadvantaged castes, raising sensation of complications during pregnancy and childbirth while promoting childbirth in health facilities contained of the occurrence of such complications and, critically, ensuring physical accessibility to the birthing facilities. In relation to strengthening health services themselves, physical facilities must urgently be improved to attract women to give birth and the skills of health workers, in particular in relation to skilled nativity attendant training, must be improved.
This cross-exclusive written report has investigated the effects of a broad range of factors on the place of commitment and has suggested some explanations on how these unlike factors exert their influence. Information technology does, however, not offer in-depth insights into the pathways affecting decision-making and how these could be addressed through public health programmes in the almost effective way. Therefore, a qualitative written report that explores in more than item how these different factors, in particular those relating to decision-making by the couple and the wider family is merited. Moreover, the effectiveness of many of the different programmes to reduce maternal deaths, including the provision of birthing centres, complimentary maternity services and financial incentives currently in place in Nepal, has not been evaluated to appointment. Their successful implementation and further improvement would benefit from high-quality operational enquiry, in particular using randomised as well every bit natural experiment studies. Much remains to be done to optimise maternal health services in an endeavour to reduce unnecessary maternal deaths in Nepal and the world.
References
-
GoN, Un. Nepal Millennium Development Goals, Progress Study, 2013. Kathmandu: Government of Nepal, National Planning Commission and United nations Country Squad Nepal; 2013.
-
WHO, UNICEF, UNFPA, The World Bank, United nations. Trends in Maternal Mortality: 1990 to 2013. Estimates by WHO, UNICEF, UNFPA, The Earth Bank and the United Nations Population Division. Geneva: World Health Organization; 2014.
-
Kerber KJ, de Graft-Johnson JE, Bhutta ZA, Okong P, Starrs A, Lawn JE. Continuum of care for maternal, newborn, and child health: from slogan to service commitment. Lancet. 2007;370(9595):1358–69.
-
Ministry of Health and Population (MOHP) [Nepal], New Era, ICF International Inc. Nepal Demographic and Wellness Survey 2006. Kathmandu: Government of Nepal, Ministry of Health and Population; 2007.
-
Campbell OM, Graham WJ. Strategies for reducing maternal mortality: getting on with what works. Lancet. 2006;368(9543):1284–99.
-
Koblinsky M, Matthews Z, Hussein J, Mavalankar D, Mridha MK, Anwar I, et al. Going to calibration with professional skilled care. Lancet. 2006;368(9544):1377–86.
-
Ministry building of Health and Population (MOHP) [Nepal], New Era, ICF International Inc. Nepal Demographic and Health Survey 2011. Kathmandu: Authorities of Nepal, Ministry of Health and Population; 2012.
-
Ministry of Health and Population (MoHP). Annual Report of Department of Wellness Services (2012/2013). Kathmandu: Government of Nepal, Ministry of Health and Population; 2013.
-
Family unit Health Division [DoHS]. Safer Mother Plan Working Guideline- 2065/2009. Kathmandu, Nepal: Family unit Wellness Division and Department of Health Services; 2009.
-
Ministry of Health and Population (MoHP) [Nepal]: Community Based Newborn Care Plan. Authorities of Nepal, Ministry building of Health and Population, Department of Health Services, National Health and Instruction, Information and Communication Heart & Child Wellness Segmentation; 2010. http://cbncp.org.np.
-
District Public Wellness Office Chitwan. Annual Health Study of Chitwan. Chitwan: District Public Health Part, Ministry of Health and Population, Authorities of Nepal; 2013.
-
CBS. Nepal in figures. Kathmandu: National Planning Commission Secretariat, Cardinal Bureau of Statistics; 2012.
-
CBS. National Population and Housing Demography, 2011. Hamlet Development Committee/Municipality. Kathmandu: National Planning Committee Secretariat, Central Bureau of Statistics; 2012.
-
CBS. National Population and Housing Census, 2011. Social Characteristics Table: (Caste/Ethnicity, Female parent Natural language and Second Linguistic communication). Kathmandu: National Planning Commission Secretariat, Key Agency of Statistics; 2014.
-
CBS. National Population and Housing Census 2011, (National Report). Kathmandu: National Planning Commission Secretariat, Central Bureau of Statistics; 2012.
-
ICIMOD, CBS/HMGN, SNV. Districts of Nepal, Indicators of Development, Update 2003. Kathmandu: International Center for Integrated Mountain Development, Primal Agency of Statistics, SNV, Nepal; 2003.
-
Babyak MA. What you come across may not be what you lot go: a cursory, nontechnical introduction to overfitting in regression-type models. Psychosom Med. 2004;66(3):411–21.
-
Bhandari Atomic number 82. Rural livelihood alter? Household majuscule, community resources and livelihood transition. J Rural Stud. 2013;32:126–36.
-
Bhandari PB, Shrestha SS, Ghimire DJ. Sociocultural and geographical disparities in child immunization in Nepal. Asia-Pac Popul J. 2007;22(ane):43–64.
-
Bennet L, Dahal DR, Govindasamy P. Caste, Ethnic and Regional Identity in Nepal: Further Assay of the 2006 Demographic and Health Surveys. Calverton, Maryland, USA: Macro International Inc; 2008.
-
Dahal DR. Social Limerick of the Population of Caste/Ethnicity and Religion. Population Monograph of Nepal 2003. Kathmandu: Primal Bureau of Statistics Nepal; 2003.
-
World Depository financial institution, DFID. Unequal citizens: gender, caste and ethnic exclusion in Nepal- Executive Summary. Kathmandu: The World Banking company and DFID; 2006.
-
Acharya M, Bennet L. The Status of Women in Nepal: The Rural Women of Nepal. Kathmandu: Tribhuvan University, Middle for Economical Evolution and Administration; 1981.
-
Pandey JP, Dhakal MR, Karki S, Poudel P, Pradhan MS. Maternal and Child Health in Nepal: The Furnishings of Caste, Ethnicity, and Regional Identity: Further Assay of the 2011 Nepal Demographic and Health Survey. Kathmandu: Calverton, Maryland, Usa: Nepal Ministry of Health and Population, New ERA, and ICF International; 2013.
-
Paudel D, Thapa A, Shedain PR, Paudel B. Trends and Determinants of Neonatal Mortality in Nepal: Further Assay of the Nepal Demographic and Health Surveys, 2001–2011. Kathmandu: Nepal Ministry of Wellness and Population, New ERA, and ICF International: Calverton, Maryland, U.s.; 2013.
-
Filmer D, Pritchett LH. Estimating wealth furnishings without expenditure Data—Or tears: an application to educational enrollments in states of bharat. Demography. 2001;38(i):115–32.
-
Lauritsen JM, Bruus M. Epi Tour: An Introduction to Validated Data Entry and Documentation of Data by Use of Epidata. Odense Denmark: The EpiData Clan; 2005.
-
Norusis One thousand: SPSS 16.0 statistical procedures companion. Prentice Hall Printing; 2008.
-
Royston P, Moons KGM, Altman DG, Vergouwe Y. Prognosis and prognostic research: developing a prognostic model. BMJ. 2009;338:b604.
-
O'brien RM. A caution regarding rules of thumb for variance aggrandizement factors. Qual Quan. 2007;41(5):673–90.
-
Wagle RR, Sabroe S, Nielsen BB. Socioeconomic and physical altitude to the maternity infirmary as predictors for place of delivery: an observation study from Nepal. BMC Pregnancy Childbirth. 2004;4(1):eight.
-
Karkee R, Binns CW, Lee AH. Determinants of facility delivery after implementation of safer female parent plan in Nepal: a prospective cohort written report. BMC Pregnancy Childbirth. 2013;13(1):193.
-
Karkee R, Lee AH, Khanal V. Need factors for utilisation of institutional commitment services in Nepal: an analysis from Nepal Demographic and Health Survey, 2011. BMJ Open. 2014;4(3):e004372.
-
Shrestha SK, Banu B, Khanom K, Ali L, Thapa Due north, Stray-Pedersen B, et al. Changing trends on the identify of delivery: why practise Nepali women give birth at home? Reprod Health. 2012;nine:25.
-
Kesterton AJ, Cleland J, Sloggett A, Ronsmans C. Institutional commitment in rural Republic of india: the relative importance of accessibility and economic condition. BMC Pregnancy Childbirth. 2010;x:thirty.
-
Anyait A, Mukanga D, Oundo GB, Nuwaha F. Predictors for health facility delivery in Busia district of Uganda: a cross sectional study. BMC Pregnancy Childbirth. 2012;12:132.
-
Kabakyenga JK, Ostergren PO, Turyakira E, Pettersson KO. Influence of birth preparedness, determination-making on location of birth and assistance by skilled nascency attendants among women in south-western Uganda. PLoS One. 2012;vii(4):e35747.
-
Danforth EJ, Kruk ME, Rockers PC, Mbaruku M, Galea South. Household decision-making about delivery in wellness facilities: evidence from Tanzania. J Health Popul Nutr. 2009;27(5):696–703.
-
Story WT, Burgard SA, Lori JR, Taleb F, Ali NA, Hoque DM. Husbands' involvement in delivery care utilization in rural Bangladesh: a qualitative report. BMC Pregnancy Childbirth. 2012;12:28.
-
Amooti-Kaguna B, Nuwaha F. Factors influencing option of commitment sites in Rakai district of Uganda. Soc Sci Med. 2000;50(2):203–13.
-
Nawal D, Goli S. Birth preparedness and its issue on place of commitment and postal service-natal check-ups in Nepal. PLoS Ane. 2013;viii(5):e60957.
-
Paul BK, Rumsey DJ. Utilization of health facilities and trained birth attendants for childbirth in rural Bangladesh: an empirical study. Soc Sci Med. 2002;54(12):1755–65.
-
Gabrysch S, Campbell OM. Still as well far to walk: literature review of the determinants of commitment service apply. BMC Pregnancy Childbirth. 2009;9:34.
-
Suvedi BK, Pradhan A, Barnett Due south, Puri K, Chitrakar SR, Poudel P, et al. Nepal Maternal Bloodshed and Morbidity Report 2008/2009: Summary of Preliminary Findings. Kathmandu: Family Health division, Department of Wellness Services, Ministry building of Health, Authorities of Nepal; 2009.
-
Ronsmans C, Graham WJ. Maternal bloodshed: who, when, where, and why. Lancet. 2006;368(9542):1189–200.
-
Teferra AS, Alemu FM, Woldeyohannes SM. Institutional commitment service utilization and associated factors amongst mothers who gave birth in the final 12 months in Sekela District, n due west of Federal democratic republic of ethiopia: a community-based cross exclusive study. BMC Pregnancy Childbirth. 2012;12:74.
-
Amano A, Gebeyehu A, Birhanu Z. Institutional commitment service utilization in Munisa Woreda, South Eastward Ethiopia: Community Based Cross-sectional Study. BMC Pregnancy Childbirth. 2012;12:105.
-
Onah HE, Ikeako LC, Iloabachie GC. Factors associated with the use of motherhood services in Enugu, southeastern Nigeria. Soc Sci Med. 2006;63(7):1870–8.
-
Mendoza Aldana J, Piechulek H, Al-Sabir A. Client satisfaction and quality of health care in rural Bangladesh. Bull Earth Wellness Organ. 2001;79(6):512–7.
-
Mpembeni RN, Killewo JZ, Leshabari MT, Massawe SN, Jahn A, Mushi D, et al. Use pattern of maternal health services and determinants of skilled care during commitment in Southern Tanzania: implications for achievement of MDG-v targets. BMC Pregnancy Childbirth. 2007;7:29.
-
Chowdhury ME, Ronsmans C, Killewo J, Anwar I, Gausia K, Das-Gupta S, et al. Equity in apply of dwelling-based or facility-based skilled obstetric care in rural People's republic of bangladesh: an observational study. Lancet. 2006;367(9507):327–32.
-
FHD. National Safe Motherhood and Newborn Health Long-Term Plan (2006–2017). Kathmandu: Family Health Division, Ministry of Health and Population, Government of Nepal; 2006.
Acknowledgements
Rajani Shah would like to thank the Farrar Foundation, Uk for its financial back up to the written report and she is besides thankful to the Nepal Public Health Foundation, Kathmandu for helping in this process. The authors are grateful to the Chitwan District Public Wellness Office, local wellness workers, female person community wellness volunteers, enumerators and participants of the study for their support and contributions.
Author information
Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
RS designed the written report, prepared the tools, managed the field work, analyzed information, and prepared the manuscript. EAR, Physician and MM contributed to decisions regarding the design and methodology of the study and offered advice during the interpretations of results. PBB advised on data analysis. All authors contributed to revisions of the manuscript and approved the last submission.
Rights and permissions
This article is published under license to BioMed Fundamental Ltd. This is an Open Access commodity distributed under the terms of the Creative Eatables Attribution License (http://creativecommons.org/licenses/past/four.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original piece of work is properly credited. The Artistic Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/one.0/) applies to the data made available in this article, unless otherwise stated.
Reprints and Permissions
About this article
Cite this article
Shah, R., Rehfuess, E.A., Maskey, Thou.K. et al. Factors affecting institutional delivery in rural Chitwan commune of Nepal: a community-based cross-sectional written report. BMC Pregnancy Childbirth 15, 27 (2015). https://doi.org/x.1186/s12884-015-0454-y
-
Received:
-
Accustomed:
-
Published:
-
DOI : https://doi.org/x.1186/s12884-015-0454-y
Keywords
- Institutional commitment
- Birthing center
- Women's empowerment
- Maternal health
- Nepal
- Southward Asia
Source: https://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/s12884-015-0454-y
0 Response to "How Is Healthcare Quality Ensured in Nepal Peer Review"
Post a Comment